
Acupuncture and Mental Health: Expert Guide to Ancient Healing for Modern Minds
There’s something counterintuitive about needles being the answer to anxiety, depression, or insomnia. Yet acupuncture, a practice rooted in traditional Chinese medicine for over 2,500 years, has emerged as a compelling complement to conventional mental health treatment. While Western medicine has long compartmentalized the body and mind, acupuncture operates from a fundamentally different premise: that mental wellbeing flows directly from physical and energetic balance.
The conversation around acupuncture and mental health has shifted dramatically in recent years. What was once dismissed as pseudoscience is now the subject of rigorous clinical research, with neuroscientists uncovering the biological mechanisms behind why tiny needles inserted at specific points can measurably reduce symptoms of anxiety, depression, and stress. This isn’t mysticism—it’s physiology meeting tradition.
Whether you’re exploring acupuncture as a standalone therapy or considering it alongside other interventions, understanding how this ancient practice works on your nervous system and brain chemistry is essential. This guide walks you through the evidence, the mechanisms, and the practical considerations for integrating acupuncture into your mental health journey.
How Acupuncture Works: The Neuroscience Behind the Needles
The traditional explanation of acupuncture involves qi (pronounced “chee”), the vital life force believed to flow through pathways called meridians. While this language might feel foreign to Western ears, modern neuroscience has begun translating these concepts into measurable physiological responses.
When an acupuncture needle penetrates the skin, it triggers several simultaneous biological events. First, there’s the mechanical stimulation of nerves beneath the skin’s surface. This activates sensory neurons that send signals to the brain, essentially “gating” pain signals—a phenomenon known as the gate control theory of pain. Essentially, your brain becomes so focused on processing the acupuncture sensation that it has less bandwidth to process other pain or distress signals.
More significantly, acupuncture stimulates the release of endogenous opioids—your body’s natural painkillers and mood regulators. Research published in peer-reviewed journals shows that acupuncture increases production of endorphins, serotonin, and dopamine, the very neurotransmitters that conventional antidepressants aim to influence. The difference is that acupuncture works through a completely different biological pathway, making it a valuable option for people who don’t respond well to pharmaceutical interventions or who experience unwanted side effects.
Additionally, acupuncture activates the parasympathetic nervous system—your body’s “rest and digest” mode. This counteracts the sympathetic nervous system’s “fight or flight” response, which is chronically activated in people experiencing anxiety, PTSD, and chronic stress. By literally shifting your nervous system state, acupuncture creates the physiological conditions necessary for healing.
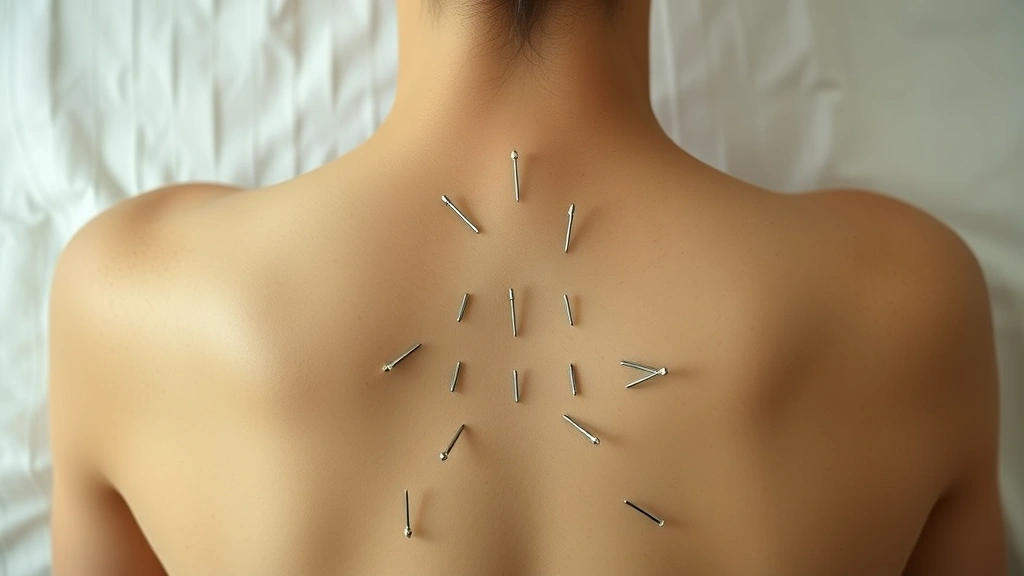
Mental Health Conditions That Respond to Acupuncture
While acupuncture isn’t a replacement for conventional psychiatric care in crisis situations, it has demonstrated efficacy for several prevalent mental health challenges:
- Anxiety and Generalized Anxiety Disorder (GAD): Multiple clinical trials show that acupuncture reduces anxiety symptoms comparable to some pharmaceutical interventions, without the sedative side effects or dependency risks. The calming effect often emerges within the first few sessions.
- Depression: Acupuncture appears particularly effective for mild to moderate depression, especially when combined with other therapeutic approaches. Some research suggests it may work as well as or better than antidepressants for certain populations, particularly those resistant to medication.
- Insomnia and Sleep Disorders: By regulating the nervous system and addressing underlying stress, acupuncture helps restore natural sleep architecture. Many practitioners report that patients fall asleep more easily and experience deeper, more restorative sleep.
- Post-Traumatic Stress Disorder (PTSD): The nervous system recalibration that acupuncture provides makes it particularly valuable for trauma survivors. It helps discharge the frozen activation state that characterizes PTSD.
- Chronic Pain with Psychological Components: Since chronic pain and mental health are deeply intertwined, acupuncture’s dual benefits on pain and mood make it especially useful for conditions like fibromyalgia or complex regional pain syndrome.
- Stress and Burnout: As a preventative tool, acupuncture helps regulate stress hormones and build resilience before acute mental health crises develop.
Understanding the stages of mental health recovery can help you contextualize where acupuncture fits within your broader healing trajectory. Some people integrate it early, while others find it most helpful during specific phases.
The Research Evidence: What Studies Actually Show
The evidence base for acupuncture and mental health has grown substantially. A landmark study published in JAMA Psychiatry found that acupuncture was significantly more effective than sham acupuncture in treating major depressive disorder. Importantly, the effect was comparable to conventional antidepressants, yet without the sexual dysfunction, weight gain, or emotional blunting that often accompanies pharmaceutical treatment.
The National Center for Biotechnology Information database contains hundreds of peer-reviewed studies examining acupuncture’s neurobiological mechanisms. Research consistently shows that acupuncture activates specific brain regions associated with emotional regulation, including the prefrontal cortex and anterior cingulate cortex.
A 2023 systematic review in Frontiers in Neuroscience synthesized 47 randomized controlled trials, concluding that acupuncture demonstrates moderate to strong efficacy for anxiety disorders and depression. Importantly, the effect sizes were clinically meaningful—not just statistically significant, but actually noticeable in people’s daily lives.
However, researchers acknowledge several limitations in the current evidence. Many studies have small sample sizes, and the placebo effect is powerful in acupuncture research (which itself is interesting—it suggests that the ritualistic, caring, and focused attention components matter significantly). Additionally, most research focuses on specific acupuncture protocols rather than individualized treatment, which is how traditional practitioners typically work.
The WHO and NIH have both recognized acupuncture as an evidence-based treatment for certain mental health conditions. While neither organization claims it’s a first-line treatment, they acknowledge it as a legitimate therapeutic option worthy of integration into comprehensive mental health care.
What to Expect: The Acupuncture Treatment Process
Your first acupuncture appointment typically lasts 60-90 minutes. A qualified practitioner will conduct a thorough intake, asking about your mental health symptoms, medical history, sleep patterns, digestion, and stress levels. This isn’t casual conversation—traditional Chinese medicine practitioners gather information that Western medicine might consider irrelevant but that informs their diagnostic approach.
The practitioner will examine your tongue and pulse, using these as diagnostic tools in traditional Chinese medicine. They’ll then explain their assessment in terms that might reference imbalances, blockages, or deficiency states in your qi. While the language differs from Western psychology, the practitioner is essentially conducting a functional assessment of your nervous system and overall physiological state.
During treatment, you’ll lie comfortably while the practitioner inserts hair-thin needles at specific points. Most people report that the insertion causes minimal pain—often just a slight pinch followed by a dull, spreading sensation called “de qi.” This sensation, while initially odd, is actually considered therapeutic. You’ll typically rest with the needles in place for 20-40 minutes while your parasympathetic nervous system gradually activates.
Many people experience profound relaxation during treatment, sometimes even falling asleep. Others feel energized afterward. The effects often build cumulatively—while some people notice immediate shifts in mood or anxiety, most benefit from a series of treatments (typically 8-12 sessions over several months) before deciding if acupuncture is helpful for their particular situation.
Those navigating active path mental health interventions often find acupuncture works synergistically with other treatments, amplifying overall benefits.
Integration Strategies: Combining Acupuncture with Other Therapies
The most effective mental health outcomes often emerge from integrated approaches rather than single interventions. Acupuncture integrates particularly well with:
- Psychotherapy: The nervous system regulation that acupuncture provides creates optimal conditions for therapy to work. Patients often report feeling more open and emotionally accessible during therapy sessions that follow acupuncture treatments. The combination addresses both the somatic (body-based) and cognitive-emotional dimensions of mental health.
- Medication: Acupuncture doesn’t conflict with psychiatric medications. In fact, many psychiatrists are increasingly open to patients pursuing acupuncture alongside pharmacological treatment. Some patients find they can reduce medication doses under their doctor’s supervision once acupuncture begins working, though this requires careful medical oversight.
- Meditation and Mindfulness: Both acupuncture and contemplative practices activate the parasympathetic nervous system. Patients who meditate often report that acupuncture deepens their practice, and vice versa.
- Exercise and Movement: Acupuncture’s benefits compound when combined with regular physical activity, which independently improves mental health outcomes.
- Journaling Practices: Exploring your mental health through journal prompts for mental health can help you track acupuncture’s effects and integrate insights from treatment into your broader self-awareness practice.
The key is viewing acupuncture not as a standalone cure, but as one component of a comprehensive mental health strategy. This perspective aligns with what the American Psychological Association increasingly recognizes: that integrative approaches combining multiple modalities often outperform single interventions.
Some practitioners specialize in what’s called “collaborative care,” actively coordinating with your therapist or psychiatrist. If your provider isn’t familiar with acupuncture, seeking out practitioners who have experience working alongside conventional mental health professionals can facilitate better integration.
Finding a Qualified Practitioner and Safety Considerations
Not all acupuncturists are equally trained. Licensing requirements vary significantly by state and country. In the United States, look for practitioners with:
- Licensed Acupuncturist (L.Ac.) or Diplomate of Acupuncture (Dipl. Ac.) credentials
- Completion of at least 1,500 hours of training (the national standard for certification)
- Passage of the National Certification Commission for Acupuncture and Oriental Medicine (NCCAOM) exam
- State licensure in your jurisdiction
When researching practitioners, ask directly about their experience treating mental health conditions. Some acupuncturists specialize in pain management; others focus on mental health and emotional wellbeing. You want someone with relevant expertise.
Safety considerations are minimal when treatment is performed by qualified practitioners using sterile, single-use needles. Serious adverse events are extraordinarily rare. The most common side effects are mild and transient: slight bruising at needle sites, temporary fatigue, or occasionally a temporary intensification of symptoms as your body begins releasing stored tension.
However, certain populations should exercise caution or avoid acupuncture entirely:
- People with bleeding disorders or taking blood thinners (though acupuncture may still be possible with modified techniques)
- Those with severe needle phobia (though many discover their fear diminishes with acupuncture)
- Pregnant individuals (though acupuncture during pregnancy is generally safe when performed by trained practitioners, certain points must be avoided)
If you’re considering acupuncture while taking psychiatric medications, discuss it with your prescribing psychiatrist. They should be supportive—integrative approaches are increasingly mainstream—though they may want to monitor your response as your overall treatment plan evolves.
Understanding common mental health care frustrations can help you approach acupuncture with realistic expectations. It’s not a magic solution, but it’s a legitimate therapeutic tool with growing evidence behind it.
For those seeking to expand their mental health literacy, exploring resources like Psychology Today’s practitioner directory can help you find both acupuncturists and therapists in your area, many of whom actively collaborate.
Frequently Asked Questions
Does acupuncture actually work, or is it just placebo?
This is the most common question, and it deserves a nuanced answer. While the placebo effect is indeed powerful in acupuncture (as it is in many medical treatments), research shows that real acupuncture produces better outcomes than sham acupuncture in clinical trials. Additionally, acupuncture produces measurable changes in brain imaging studies—we can literally see activation in specific brain regions. That said, the ritual, attention, and therapeutic relationship surrounding acupuncture contribute meaningfully to outcomes. This isn’t a weakness; it’s actually a feature. Effective treatment often involves multiple components working synergistically.
How many sessions will I need?
This varies considerably depending on your condition and individual response. For acute anxiety or stress, some people notice shifts within 1-3 sessions. For chronic conditions like depression or PTSD, a typical course involves 8-12 sessions over 2-3 months, with reassessment at that point. Some people benefit from ongoing maintenance sessions monthly or bi-monthly, while others achieve their goals and discontinue treatment. Your practitioner should establish clear benchmarks for evaluating whether acupuncture is helping your particular situation.
Can I use acupuncture instead of medication?
This is a decision to make collaboratively with your mental health provider, not independently. For mild to moderate anxiety or depression, some people find acupuncture sufficient as a standalone treatment. However, for severe depression, bipolar disorder, schizophrenia, or acute suicidality, medication is typically essential. The most effective approach for many people is combining acupuncture with medication, potentially reducing medication doses over time under medical supervision. Never discontinue psychiatric medication without your doctor’s involvement.
What does “de qi” feel like, and is it necessary?
De qi is the sensation of heaviness, warmth, or spreading numbness around the needle site. It’s considered therapeutic in traditional Chinese medicine, and many practitioners aim to elicit it. However, you shouldn’t experience sharp pain. If you do, let your practitioner know immediately—they can adjust needle depth or location. De qi enhances outcomes but isn’t absolutely required for benefit. Some people never experience pronounced de qi and still improve significantly.
How does acupuncture compare to antidepressants?
Research suggests they’re roughly comparable in efficacy for mild to moderate depression, though acupuncture has a different side effect profile. Antidepressants work faster (2-4 weeks) but often cause sexual dysfunction, weight gain, or emotional blunting. Acupuncture works more gradually but without these side effects. Many people prefer trying acupuncture first or combining it with lower medication doses. The best choice depends on your individual situation, severity of symptoms, and personal preferences. This is worth discussing with both your psychiatrist and acupuncturist.
Is acupuncture covered by insurance?
Coverage varies widely. Many insurance plans now cover acupuncture for pain conditions, and some specifically cover it for mental health. Call your insurance provider with your policy number to ask about coverage for acupuncture related to your specific condition. Some practitioners offer sliding scale fees if insurance doesn’t cover treatment. Don’t let cost concerns prevent you from exploring acupuncture—many communities have community acupuncture clinics offering affordable treatment.
Can I combine acupuncture with therapy?
Absolutely—this combination is often ideal. Acupuncture regulates your nervous system, creating optimal conditions for therapeutic work. Many therapists actively encourage clients to pursue acupuncture. If you’re considering both, you might schedule acupuncture appointments shortly before therapy sessions to maximize the benefits of both. Ideally, your acupuncturist and therapist would be aware of each other’s involvement and could coordinate care.
What credentials should I look for in an acupuncturist?
Look for Licensed Acupuncturist (L.Ac.) or Diplomate of Acupuncture (Dipl. Ac.) credentials, verification of state licensure, and confirmation that they’ve completed at least 1,500 hours of training and passed the NCCAOM certification exam. Ask about their specific experience treating mental health conditions and whether they’re open to collaborating with your other healthcare providers. Word-of-mouth recommendations from therapists or other healthcare providers can also be valuable.


